Discovering the possibilities of future surgery
We are constantly improving surgical techniques through research, investigation and innovation.
Since The Baird Institute’s inception in 2001 we have funded clinical trials, PhD students, surgeon scientists, laboratory work, surgical training, research into surgical outcomes and digital imaging research.
Through this research, and the partnerships we have forged, The Baird Institute is now a recognised and established international voice in the field of cardiothoracic surgical research.
Ultimately, The Baird Institute facilitates connection.
It is a stellar example of how a small cohort of surgeons working in conjunction with undergraduate and postgraduate Faculties of Medicine, can work to improve surgical techniques, materials and evidence-based care, to enhance the quality of patients’ lives.
We are currently furthering the fields of heart and lung surgery by:
- Developing innovative techniques for better heart valve surgery
- Conducting advanced research into the use of robotic technologies in order to speed up diagnosis and improve future treatment possibilities
- Supporting the use of the Kuka – a new robotic arm to be used in surgery
- Establishing three robotic databases – Robolung database, Robocab database and Robomitral database – to collect details regarding robotic surgery. Data is collected on the procedure itself as well as patient quality of life after surgery.
- Supporting the introduction of robotic surgery into the public hospital system
- Working with others to create innovative techniques for imaging blood flow, to determine the cause of Aortic Aneurysm Disease.
- Conducting innovative research into how the heart/lung machine affects organ function during open-heart surgery and how to make it more effective and safer
- Collecting data and analysing both illness patterns and the effectiveness of our work
It is an exciting time for The Baird Institute and we invite you to be a part of our ambitious future.
After laying all the right foundations, we’re now at the point where we can start delving into the possibilities that robotics, nanorobotics and digital imaging can create for research and surgical practice; particularly in the areas of cardiac disease, biological studies and genetic disease.
We believe that these directions in investigation will ensure that The Baird Institute remains an international leader in translational research, the translation of evidence into public health practice and policy; thus enabling cutting edge research to rapidly result in improved cardiothoracic surgical practice.
The Baird Institute does not receive any government funding and relies solely on the generosity of the public and those who have benefited from its work.
Your support will make these world-leading investigations possible.
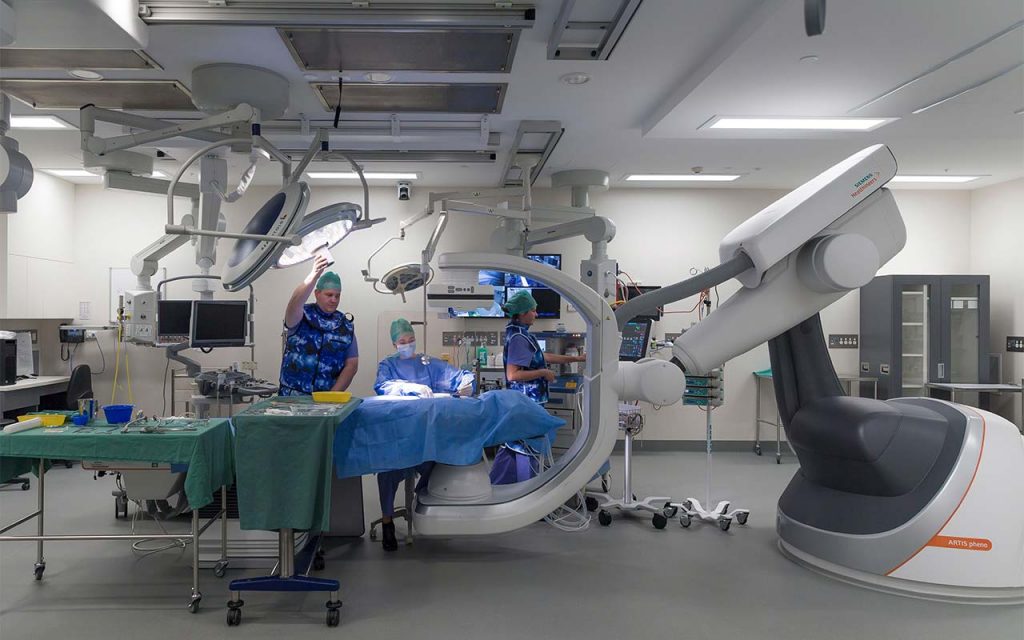
The Hybrid Theatre - On the Edge of Tomorrow
The cardiothoracic surgeon of the future is a hybrid of surgeon and research scientist while the operating theatre of the future is a hybrid theatre, a facility where high level imaging, robotics and traditional surgical procedures are combined to produce the best outcomes. The equipment at the Hybrid Theatre, in the Charles Perkins Centre (CPC) at the University of Sydney, where much of our research takes place, is the best in the world. It is a facility where researchers, clinicians and industry partners come together to rapidly translate evidence into state-of-the-art clinical practice.
Some of the best researchers in the world reside in Australia and, without a doubt, this is the best place for them to imagine, contemplate and investigate the possibilities of the future. At the CPC, the only limit to what they can achieve is their imagination.
Robotic Surgery
Robotic-Assisted Thoracic Surgery
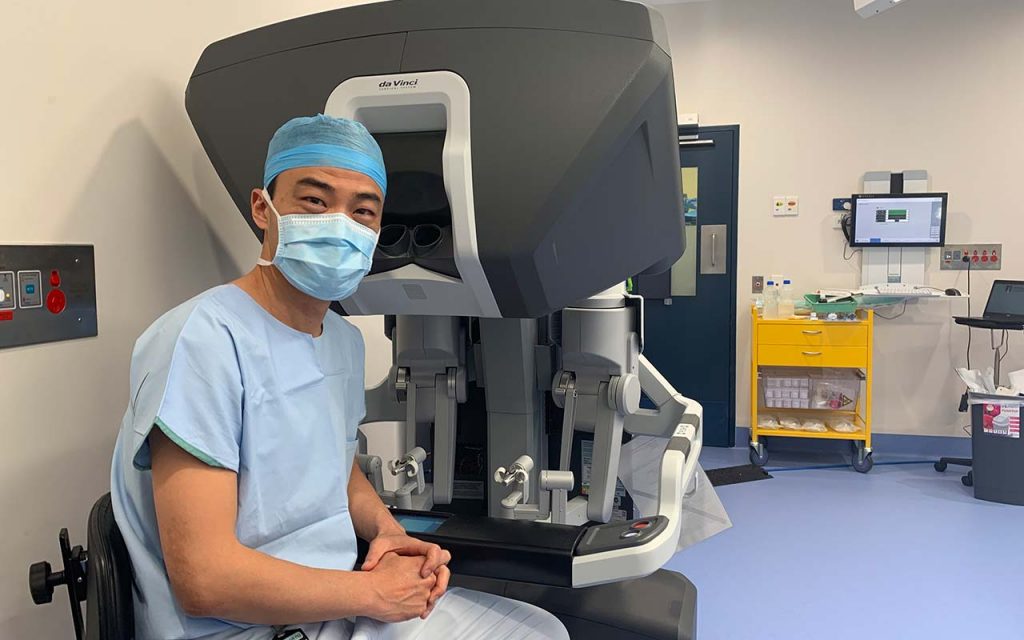
Dr Tristan Yan, cardiothoracic surgeon and his team have started the public thoracic da Vinci surgical system program at Royal Prince Alfred Hospital. The sophisticated robotic device gives the surgeon access inside the chest cavity through tiny incisions and provides improved visualisation, better access to mediastinal tissues and improved ability to remove lymph nodes as part of a cancer operation. Compared to surgery performed through a 20cm open-chest incision, robotic thoracic surgery provides several benefits for patients including; faster recovery and return to normal activities, shorter hospital stay, less pain, reduced scarring and minimal blood loss. Professor Tristan Yan, acquired the robotic surgical skills from the United States and is one of the few surgeons who can perform a robotic lobectomy in Australia. Doctor Yan received the inaugural Slater & Gordon Mesothelioma Fellowship in 2008, from The Baird Institute, which enabled him to complete his Master of Surgery in 2010
Minimally Invasive Robotic-Assisted Thoracoscopic Surgery
Associate Professor Chris Cao
Minimally invasive robotic assisted thoracoscopic surgery has evolved as a safe and efficacious procedure for patients with lung and pleural diseases in the United States and Europe. Through small incisions, surgeons are able to control a variety of instruments to excise lung and mediastinal cancers with three-dimensional magnified vision, seven degrees of freedom of movement and increased precision with reduced tremor. Associate Professor Christopher Cao has led a team of leading international thoracic surgeons and medical lung cancer specialists to establish the largest international database to date to study the safety of robotic surgery for patients with lung cancer. These studies were conducted in “Memorial Sloan Kettering Cancer Center” in the United States, the largest cancer institution in the world. In addition, the studies were published in three top international journals in 2019. With support from The Baird Institute, we are analysing our own surgical results from Royal Prince Alfred Hospital to improve the clinical outcomes of patients who undergo robotic cardiothoracic surgery. Our aim is to deliver cutting edge technology to minimize risks to patients, shorten hospital stay, reduce pain, and improve quality of life
Robotic Mitral Valve Repair
Professor Tristan Yan
There has been tremendous evolution and innovation in cardiac surgery. In the early years of the specialty, innovation focused on decreasing mortality and expanding the pathologies that surgeons could address during heart operations, while in the current era, with operative mortality for routine procedures exceedingly low, the focus has shifted to decreasing perioperative complications, improving perioperative quality of life, and maximizing long-term outcomes. As a result, the onus has fallen on surgeons to shift away from the traditional sternotomy (a type of surgical procedure in which a vertical inline incision is made along the sternum, after which the sternum itself is divided) and offer equally effective operations through less invasive approaches.
In 2019, Professor Tristan Yan was appointed as the clinical lead of the Minimally Invasive and Robotic Cardiothoracic Surgery Program at RPAH. He has performed more than 1000 minimally invasive cardiothoracic procedures with excellent clinical outcomes.
To enhance the RPAH Minimally Invasive Cardiothoracic Surgical Program, Professor Martin Misfeld, the co-director of Leipzig Heart Centre (Europe’s largest cardiac centre) was also appointed as a senior cardiac surgeon at RPAH. Together, they performed the first robotic mitral valve repair at RPAH. “Mitral valve surgery is one area that has seen some of the most impressive progress over the last two decades. With the advent of new technology, including peripheral cannulation systems, specially designed instruments, and robotic-assistance, complex valve repair and replacement can now be performed through small access incisions in the right chest without disturbing the skeleton. Minimally invasive surgical approaches offer patients gold standard results with fewer complications and a faster recovery, ensuring that despite the growth of transcatheter technologies, patients and cardiologists will not have to make the choice of trading long-term efficacy for short-term gains”, said Professor Misfeld.
One of the research projects currently under investigation is examining the advantages of minimally invasive surgery including less bleeding, enhanced cosmesis, shorter ICU and hospital length of stay, better respiratory function, less transfusion requirements, less infectious complications and faster return to work. The project also analyses the possible complications and the reasons for the robotic approach not gaining widespread use, which may include the complexity of procedure, and the cost associated with greater initial investment, maintenance, disposable instruments and retrograde cardioplegia catheters. In the study, it has been suggested that this may be compensated for by the overall economic advantages of a robotic approach, specifically shorter hospital stay and faster return to work.
The available literature has clearly shown that the costs associated with robotic-assisted mitral valve surgery are in no way prohibitive. The potentially increased costs relative to traditional approaches are easily offset by the many advantages of the evolving technology. Given the present cost-conscious healthcare climate, the appraisal of the economics of robotic surgery, supported by The Baird Institute will only intensify and, as adoption broadens and more surgeons become facile with the technique, the balance will likely continue to move in favour of this impressive technology. Future robotic mitral operations will be customized for each patient and will be based on their valve pathology, comorbidities, fragility, and age as well as their surgeon’s ability. The less invasive era in cardiac surgery is here, we need to keep an open mind and adapt to change!
More operations done using robotic surgery
Surgeons and robots team up in more hospitals
“What we always do is try to work out some way of doing things better,” says Professor Bannon. “The surgical paradigm right now is minimal invasiveness. Robots are already helping us do that.
Minimal invasiveness means faster recovery for patients with the added benefit of freeing up hospital beds.”
The da Vinci Surgical System is descended from robotic technology developed by the US military in the ’80s and ’90s that was designed to operate on soldiers on the battlefield. It has been used in hospitals in Australia since 2003. There are now six at the Royal Prince Alfred Hospital and on the University of Sydney campus, including in the Hybrid Theatre, which is the most advanced unit of its kind in the country.
While robotic surgery is fulfilling its immediate potential, Professor Bannon, Associate Professor Thanigasalam and other clinicians working in the area are mapping out the technology’s future, “The next question is whether we can go hands-off so robots operate by themselves,” says Professor Bannon. “Beyond that, can robots actually make decisions? We’re in the process of learning what the machine can learn.”
Professor Thanigasalam commented ; “For the last 100 prostate cancer operations we have performed across the Royal Prince Alfred and Concord Repatriation Campus, we found that robot surgery meant less blood loss, shorter hospital stays and less opioid usage compared to open surgery.”
If robots can one day make clinical decisions, it will be through machine learning which is related to artificial intelligence. Once provided with vast amounts of relevant information – in this case, the performance of countless surgical procedures – the da Vinci system has the capacity to work out how to do the procedures autonomously. This is where humans may have to adjust expectations in being comfortable with a machine making clinical decisions. Though in some ways, this is already happening. Some pacemakers now have a robotic element that monitors blood chemistry and fags when treatment may be needed. People who have diabetes also benefit from semi-autonomous devices assessing glucose levels and making decisions about insulin doses. “Though actually, robotic systems don’t make decisions,” points out Professor Bannon. “They draw conclusions based on vast amounts of data that have been implanted. How far we can take this will be defined by the safety nets we put in place. And the safety nets will always be multi-layered and extensive.”
While fully autonomous robotic surgeons are still some time off, Associate Professor Thanigasalam sees a variation happening sooner, “Robotics could act as a fail-safe by overriding a surgeon in case of error. Then within maybe 20 years, we’ll likely see artificial intelligence within robotics,” he says. Much more imminent is remote proctored robotic surgery. This is where a surgeon new to the technology in say, Wagga Wagga, can be supervised by a robotic surgeon in Sydney, and guided along the robotic surgery learning curve. With the horizons of robotic surgery widening, previously ambitious goals become achievable. As Professor Bannon says, “If you don’t set objectives, you’ll never know what’s possible.” Certainly, the Hybrid Theatre is working towards becoming part of the global development of new technology in surgical robotics.
Extract from the article “More operations done using robotic surgery” . Originally published in the University of Sydney’s SAM (Sydney Alumni Magazine) on 2 April 2019
Written by Gabriel Wilder. Photography by Stefanie Zingsheim
Imaging Technology
Surgeon and Professor Paul Bannon (chair of The Baird Institute), and fellow board member and cardiologist, Richmond Jeremy are working with Professor Grieve (a scientist and Radiologist) at the Charles Perkins Centre to investigate blood flow in the abnormal ascending thoracic aorta, with the assistance of a National Health and Medical Research Council (NHMRC) grant. This research blends with studies made possible due to the establishment of an Aortic Tissue Bank and Database at Royal Prince Alfred Hospital; allowing research into cardiac disease processes and surgical care.
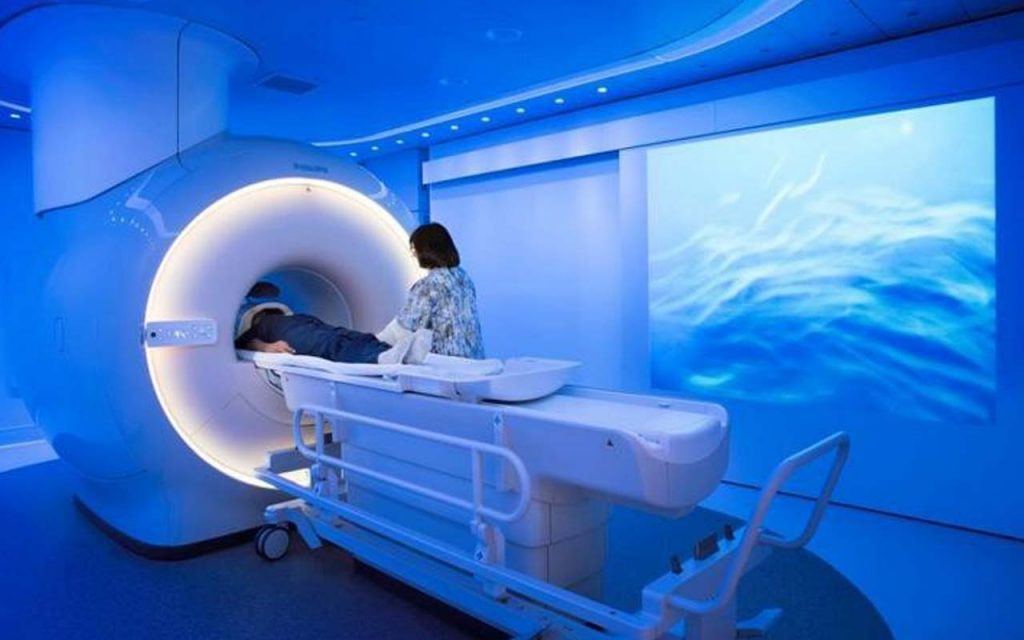
An imaging analysis known as Neural Connectivity, is being undertaken by Professor Grieve and colleagues, to explore imaging processes to better understand brain injury after cardiac surgery. New imaging technologies using MRI are now able to identify subtle brain injury not seen using other imaging technology.
This is exciting, ground-breaking work, recently published in the British Journal of Anaesthesia, 2017: ‘Neural network imaging to characterize brain injury in cardiac procedures: the emerging utility of connectomics’.
In addition to this form of imaging, the use of computational modelling and augmented reality for surgical planning and teaching is now becoming part of tertiary-level practice. 3-D printing and bio-printing are proving to be important to research as is the understanding and production of biomaterials, currently being explored with our affiliate researcher, Dr Steve Wise.
Studies are investigating coronary artery bypass grafting, and other forms of cardiac surgery, which may be associated with silent brain injury (SBI). Using MRI studies, neuronal connectivity is being explored to better understand and investigate brain injury that is not immediately evident and is sub-clinical in nature. Both on-pump (using cardio-pulmonary bypass oxygenation) and off – pump cardiac surgery techniques will be included in the study design. For those patients who require valve surgery, percutaneous and open techniques will be compared.
Virtual Reality - Vantari VR
The Baird Institute is working with Vantari VR to build a virtual reality tool for surgical planning. The focus is on improving efficiency and outcomes for patients and is the first of its kind globally to be built for use in aortic surgery. The potential of this technology is game-changing to the surgical landscape. Vantari VR is developing core technology which takes CT & MRI scan data and converts it into 3D models in the virtual reality (VR) environment, ie. it will be made visible through 3D googles.
Vantari’s aim is to build a system which will not only scan and assess acutely ill patients within minutes on the operating table, but also allow surgeons to take a virtual reality tour inside the patients’ bodies in real time; thus enabling them to plan the surgery required with much greater speed and accuracy. Clinical trials are already showing that VR can reduce surgical planning time by up to 40% and increase surgical accuracy by 10%.
“The work we are doing with Professor Bannon is for surgical planning of aortic dissection surgery,” said Dr Vijay Paul, Co Founder of Vantari VR.
“We take preoperative aortic dissection patients’ scan data which is then manipulated within our software. The software provides the 3D render but also has powerful algorithms, tools, user interface and overlay functions which allows the surgeon to plan the surgery in a way that has never before been done before.”
The software will be used in the pre-op setting but ultimately the vision is for implementation within the Hybrid Theatre setting with the MRI machines. The intra-operative (during the operation itself) imaging done on the MRI machines will also be run through Vantari’s VR software and converted into 3D renders so that a surgeon can then adapt the plan that was done up prior to surgery.
“Patients will have preoperative scans and a surgical plan within our software prior to surgery, but in the Hybrid Theatre they will be able to have on-the-table imaging mid-surgery and review within our software again. This will happen down the line as data is gathered and we go through the regulatory pathway” said Dr Paul.
Where does our focus on innovation come from?
The namesake of The Baird Institute, the late Professor Douglas Baird AM (1940- 1995), was a gifted cardiothoracic surgeon and Head of the Cardiothoracic Surgical Unit at Royal Prince Alfred Hospital.
Professor Baird believed firmly that surgical outcomes needed to be continually measured and improved.
Professor Baird was dedicated not just to improving patients’ survival rates and lives post-surgery; but to providing much needed support for surgeons and education for students.
He was instrumental in creating the first national cardiac surgical database, with the National Heart Foundation, so that lessons from past surgeries can now be implemented into current and future technologies. Though this may seem logical, it had not previously been done at the time.
Professor Baird also pioneered the formerly rare combination of research and surgery; thus bridging the gap between academic innovation and applied cardiothoracic surgical techniques.
With your help The Baird Institute can continue Professor Douglas Baird’s life-saving work and research, driving medical breakthroughs in heart and lung surgery.
To achieve our goals, push the boundaries of today and realise the possibilities for future surgery, The Baird Institute needs to guarantee funding for our team.