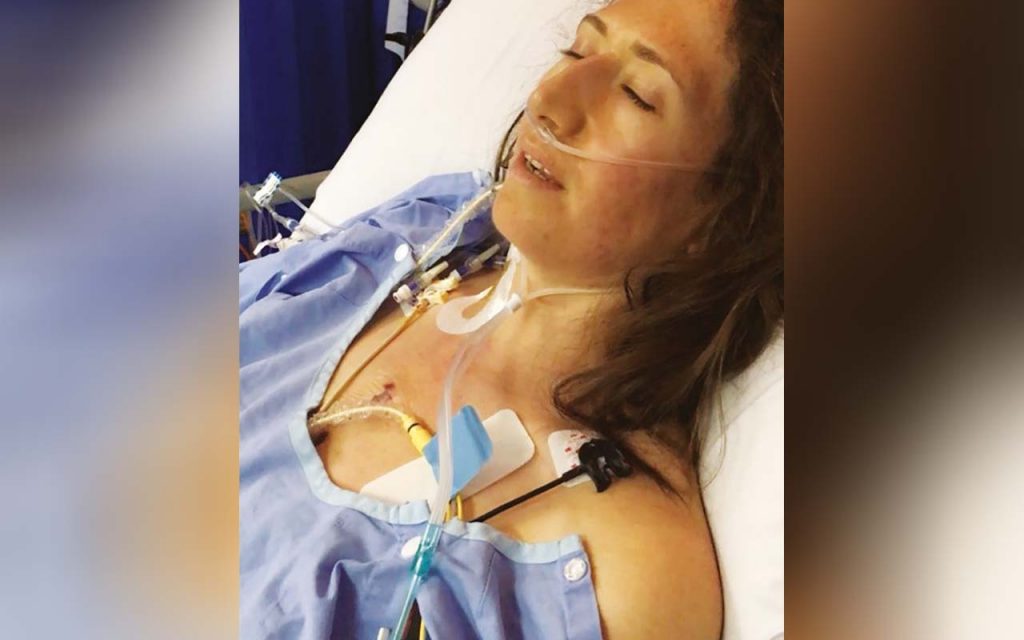
My name is Rebecca Mason and I have Marfan Syndrome
For you, the 9th of October 2018 may have been a run-of-the-mill forgettable day – get up, coffee, work, light exercise, dinner, family time. The usual. But for me, it was the day, at age 31, that I underwent open-heart surgery.
Flashback to 1989 and I had just turned 2 years old. I kept running into glass doors and Mum questioned my eyesight, or lack thereof. She waltzed into the ophthalmologist’s office, aiming for a glasses prescription before we’d head to David Jones for lunch. Instead, she was being handed documents and scripts to take me to the Children’s Hospital. Dr Martin had calmly highlighted he suspected I had Marfan Syndrome – a connective tissue mutation where the most fatal aspect of Marfans involves the heart.
I remember well the run-down lime-green walls of the old Children’s Hospital in Camperdown. Dr Martin had been on the money all from a simple eye exam. The tests came back confirming I had Marfan Syndrome. We never made it to David Jones that day.
The Red Zone
With Marfans, the aorta is about twice the size of an average person’s. The biggest risk is that if it doesn’t stop growing, it ‘dissects’ (splits in half) with a high chance of fatality. To reduce the chances of that happening, open-heart surgery is required to spare the valve.
Every year since I was 2, I had been monitored annually. Hooked up to echocardiograms and the growth of the aorta measured until I’d reach that at risk ‘red zone’. I’d somehow made it to 30 without needing the jaws of life, but stats showed it was just around the bend.
I figured if I could train my physical and mental bodies it would help me to prepare for the worst-case scenario should it hit. My regimen involved a personal trainer, Saturday pump classes, long distance ocean swimming, mindset coaching, a nutritional program and advice from an estate planner on how to structure my finances if I did pass away. About 18 months into this regime my cardiologist found a minor growth and decided we’d need the surgery in a matter of weeks.
Before I knew it…
It was the night before my operation. After having the last full meal I’d eat in 10 days I started my first round of sedation medication. Little did I know it was the last time I’d be able to lie down flat on my back for 3 months without feeling like a knife was going through my torso and swing my legs over the bed without a rope. Or laugh, or give a hug without feeling like my chest would burst in half.
"It is because of the Institute’s research and investment in technology that I’m alive today"
I woke up the next day, had my antibacterial shower and said my final goodbyes to my family and was hooked up to oxygen.
I was carted into the preoperative theatre and the nurses kindly told me I’d experience a bit of tingling in my left arm…That’s the last conscious moment I remember with my old heart.
Everest
Something must have gone well, because I woke up in ICU. Everything about my physical body was immobile leaving nothing but my eyes and lips that could move freely without support or excruciating pain.
By the next day, I hadn’t slept for about 48 hours, eaten anything for 3 days and the anaesthetic and horse-tranquiliser pain medication had made its last run.
I felt like I had been hit by 10 semi-trailers and like Mt Everest was growing from my neck to my navel, it was pain like nothing I’d ever known. The medication in itself was sickening, and I could hardly keep it down. The weight of the excess fluid was taking its toll, I was now 10kgs heavier and I hadn’t moved in days. I could feel my lungs heaving, every breath felt like I was lifting bricks in my back and my body had gotten so heavy not having moved. I was covered in tubes and drains from across and down my neck, across, underneath and in my ribcage and drips down both arms. I wanted to cry from the pain, vomit from the medication and collapse from exhaustion, I had nothing left in my tank. I felt depleted. Empty. Beaten up. This was the test that all the training had prepared me for.
The next 3 hours were the longest, toughest and most excruciating minutes of my life that felt like days. My Mum and Sister were at the end of my bed, experiencing a world of pain of their own, watching me fade. They put on a brave face, making light jokes and making sure I knew that they loved me. I couldn’t speak or return their messages of love. Mum said she just heard my screams looking into my eyes.
And then some sort of miracle happened. The nurse said I was getting better quickly, and they could move me out of ICU into my own room…much much quicker than they had expected. I had no idea what had happened, all I knew was that I was out of the risk-zone, and I could finally sleep without worrying I might not wake up again. I slept for pretty much 4 days straight after that. It wasn’t exactly easy afterwards, but I knew the worst was over.
I am incredibly honoured, and humbled to write my story for The Baird Institute. It is because of the Institute’s research and investment in technology that I’m alive today. You could say (prepare for a bad pun) that’s it’s close to my heart! It’s also the reason that in a few years’ time, anyone going through this experience may not need their chest broken, but a small incision will suffice.
This is the profound impact scientific research and technology can have on the lives of us that can’t escape open-heart surgery, so please support The Baird Institute’s 2020 Mid-Year Appeal.