Research Update – September 2023
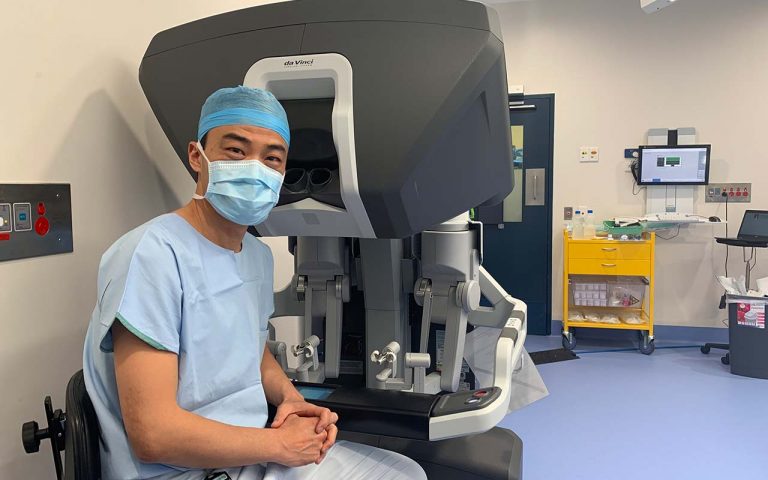
I have been researching now with the kind support of The Baird Institute for just over a year and have sincerely enjoyed my time thus far. As microscopic analyses are my forte, I have been helping across multiple research projects by imaging cardiac tissue at high magnifications using specific fluorescent markers, as well as performing…